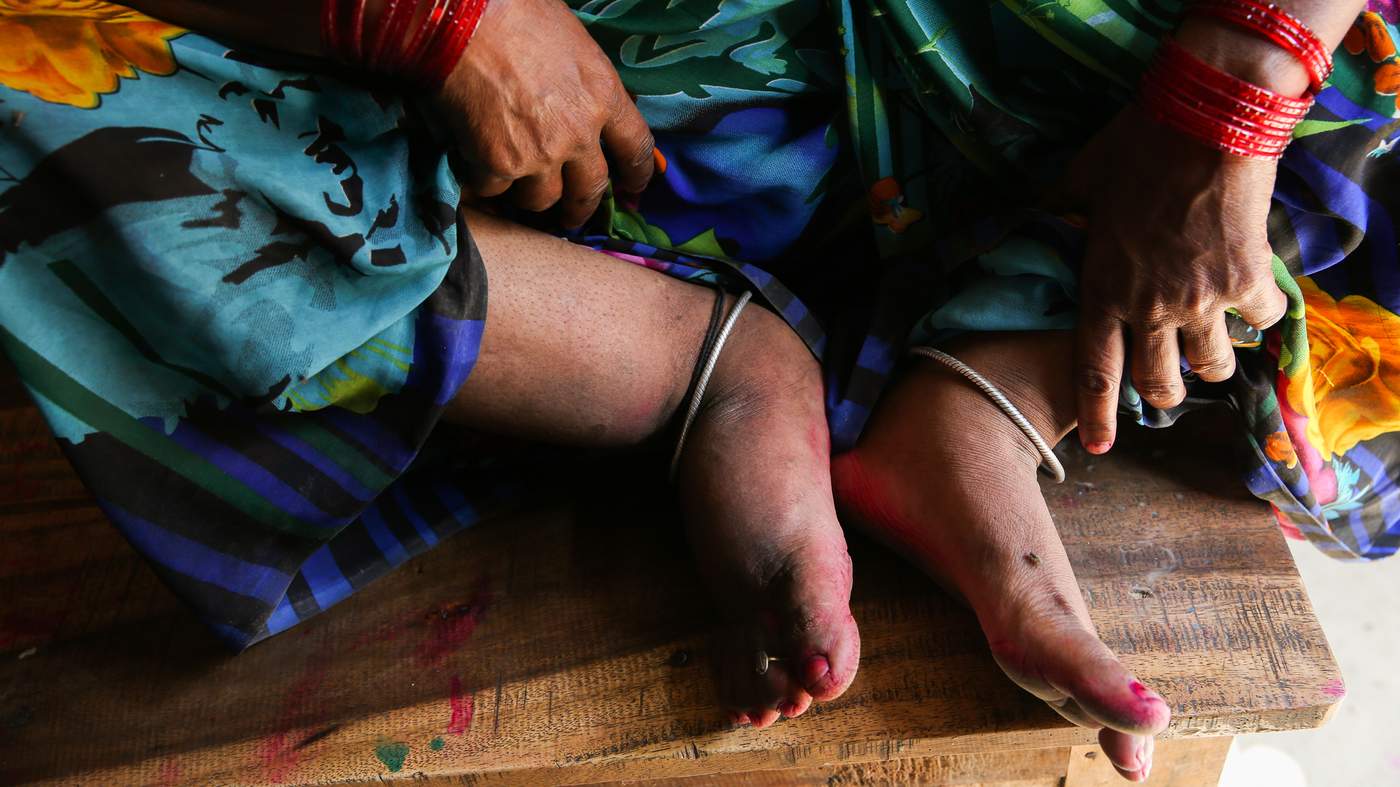
Subhash Chandra Chaubey was 14 years old in 1981 when his right leg began to swell. At first the change was almost imperceptible but, in the years that followed, it grew bigger and more deformed. Today, his leg resembles an elephant’s, with thick skin and a bloated foot.
Chaubey’s misshapen limb is a tell-tale sign of lymphatic filariasis, also known as elephantiasis, a neglected tropical disease caused by a mosquito-borne parasitic worm that lodges inside the body and disrupts the lymph system.
The damage — typically concentrated in a leg or arm, or sometimes in the groin and genitals — disrupts the normal circulation of lymphatic fluid, which then pools in the affected tissue. It leaves the affected areas vulnerable to severe infections from even the most minor scratches or abrasions, especially in rural villages, where sanitation can be poor.
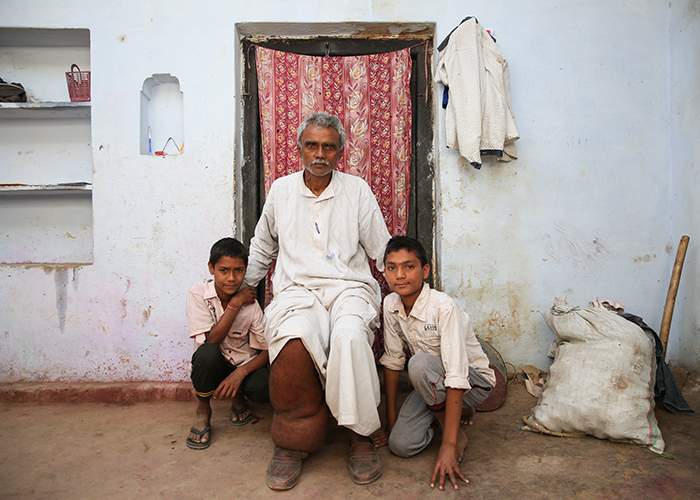
Chaubey with his two sons outside his home
Over time, repeated infections, which cause high fevers in the sufferer and lead to the extreme swelling of the limb and thickening of the skin, have severe economic and social consequences for people affected and their families.
“I am a burden,” says Chaubey, who is now 52. “No one wants to have me around.”
As a young man, Chaubey supported his family by farming the land he inherited from his father in the village of Seur in the northern state of Uttar Pradesh. In those days he could ignore the discomfort of his slightly swollen leg.
Today, however, the weight and shape of the limb makes it too exhausting to tend to his land. “In this condition, I cannot walk at all,” he says. “If you ask me just to walk across to the main highway, I would be exhausted.”

Chaubey bicycles to work as a nightwatchman
Instead, in the evening, he gets on his bicycle and pedals 1km to a shop that sells cooking gas cylinders, where he works as a nightwatchman, earning Rs3,000 (about $47) a month to help support the four of his five children who are still living at home. His land has been leased to tenant farmers, bringing in some additional income.
In a quest for a cure, Chaubey has travelled to hospitals across India, including in New Delhi and Mumbai, but none could offer him any help. At this late stage of the disease, the damage to the limb cannot be undone but only managed, to try to prevent recurring infections that could further deform the leg.
“Whenever I went for treatment, there was no medicine to cure it,” Chaubey says. “Nothing worked.”
Chaubey describes the fevers he suffers as a result of frequent infections in his affected leg
Today, Chaubey’s main anxiety is about how his disfigurement affects his children. “They face embarrassment,” he says.
Money is also a problem. His eldest daughter, who is 21, was married last year and moved to live with her husband’s family. Chaubey borrowed Rs300,000 to pay for the wedding but he still has another two daughters, aged 18 and 16, as well as two sons, 14 and 11, to worry about.
“If someone looks at me, once they see, they turn their faces away,” he says quietly. “Nobody wants to see this. People say a lot of things — I just have to swallow that. God has given me this disease and I have to suffer and live with it.”
Lymphatic filariasis, known in Hindi as hathipaon — literally, elephant-foot — is estimated to affect about 120m people in Asia, Africa, Pacific islands and parts of South America and the Caribbean. Of those affected, about a third are living with visible signs of the disease.
The distinctive symptoms have been described in art and literature for millennia. An ancient Egyptian statue depicts Pharaoh Mentuhotep II, who ruled 4,000 years ago, with swollen lower legs and feet.

Pharaoh Mentuhotep II (who reigned c.2055-2004BC) was depicted in statues with swollen lower legs and feet
The Greeks and Romans described patients with the symptoms and the Indian physician Sushruta referred to a disease he called shleepada — Sanskrit for elephant foot — in a medical treatise written in around 600BC.
In the 16th century, Jan Huygen van Linschoten, a European explorer of India’s western coast, observed that the inhabitants were “all born with one of their legs and one foot from the knee downwards as thick as an elephant’s leg”. Explorers in other parts of Asia and Africa gave similar accounts.
It was not until the second half of the 19th century that scientists discovered the threadlike worms that cause the disease and gradually pieced together the parasite’s complex life cycle and how it could spread from person to person through a mosquito bite.
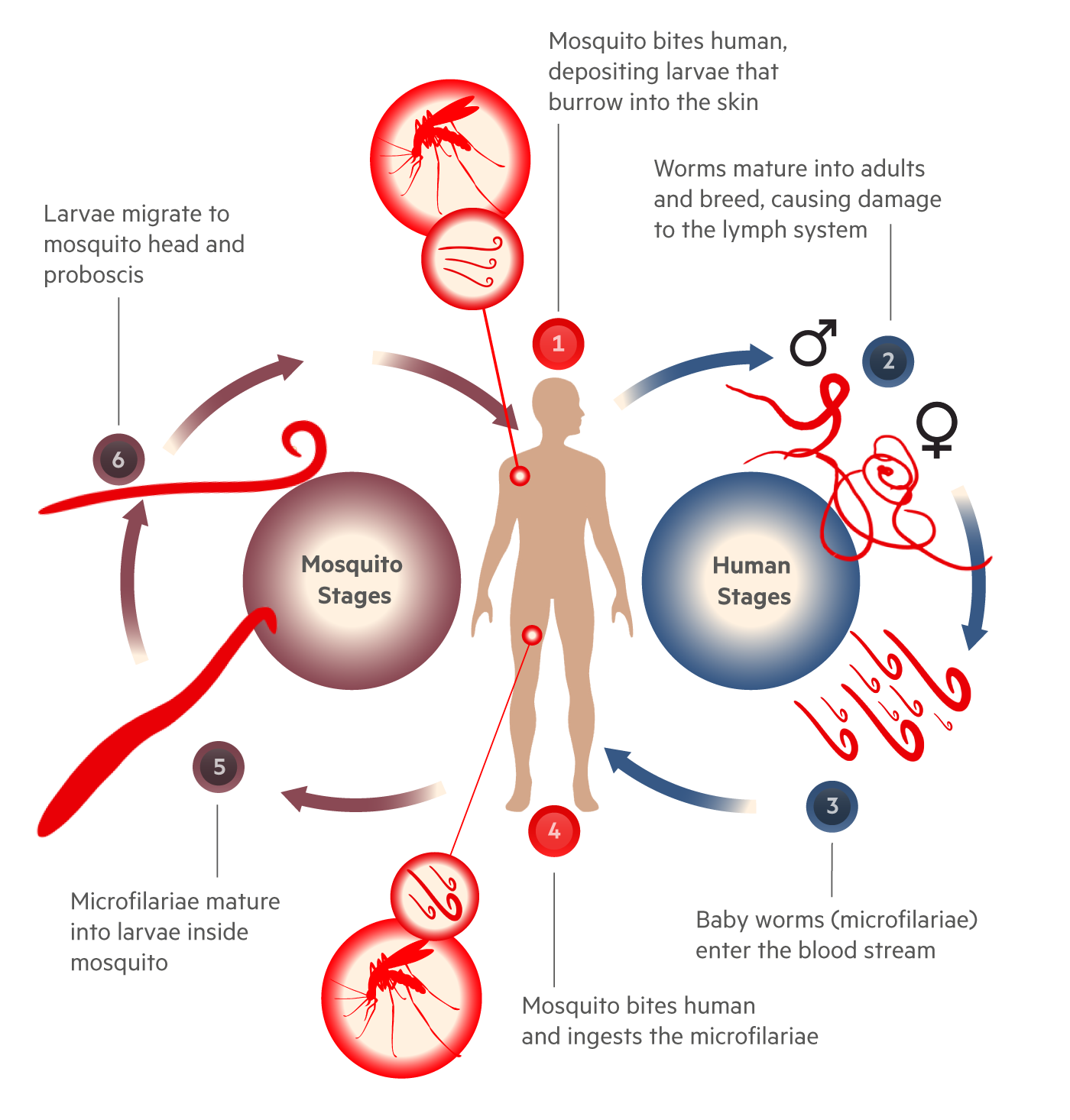
Life cycle of the parasite that causes lymphatic filariasis
The adult worms that do the damage to the lymphatic system can live inside their human hosts for several years. During this time they breed, producing tiny, threadlike baby worms, or microfilaria, that course through the bloodstream. Mosquitoes ingest the microfilaria when they bite an infected person and the baby worms remain inside the insects for about two weeks, growing into bigger larvae. When the mosquitoes bite again, those more mature larvae are deposited on to human skin. They burrow into the new human host and grow into adults.
Efforts to fight mosquito-borne diseases usually include exterminating the insects or trying to prevent them from biting humans. But, in the case of lymphatic filariasis, public health programmes are instead focusing on killing the parasites inside their human hosts.
This is not an easy task. It requires a process known as “mass drug administration” — persuading the entire population of an affected area to take medication, whether they show symptoms or not. For lymphatic filariasis, the medicine comes in the form of deworming drugs, which must be taken once a year, every year, for five consecutive years — the estimated reproductive span of the adult female worms.
The World Health Organization is determined to stop the spread of lymphatic filariasis, which is present in 73 countries. It has set the world a goal of eliminating the disease by 2020.
“Elimination” means bringing prevalence down to less than one case per 10,000 people in an endemic area. The ultimate goal — eradication — would mean reaching the point where there is no possibility of the disease occurring anywhere in the world. In human history, only one disease has successfully been eradicated: smallpox.
Despite the difficulties, some countries have been successful. China and South Korea were declared filaria-free a decade ago. The Maldives, Sri Lanka, Cambodia and three Pacific island nations achieved the goal in 2016. In April this year, Togo became the first sub-Saharan African country to rid itself of the disease. Eighteen more countries have completed five years of mass drug administration and are performing surveillance programmes to confirm the disease has been stopped in its tracks.

A poster for Filaria Awareness Day on a wall outside a hospital in Bhadohi, Uttar Pradesh
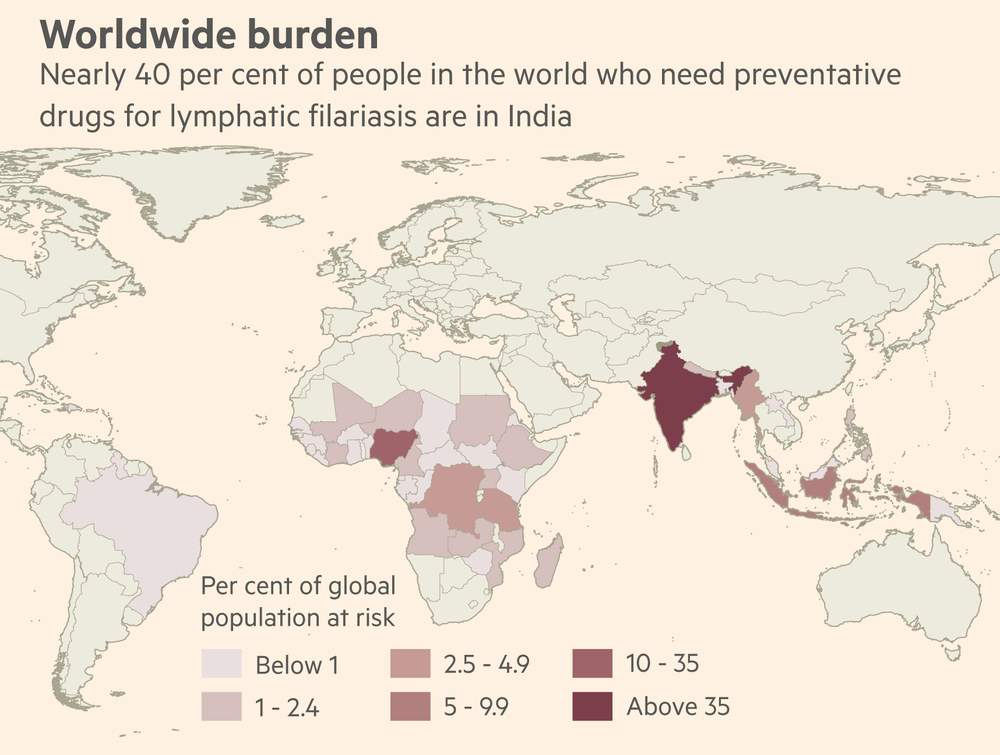
India is a crucial battleground: home to almost 40 per cent of those who are infected and need treatment, according to estimates from the World Health Organization — more than triple the next most affected country, Nigeria.
Officially, New Delhi has set a goal of eliminating the disease by the end of this year. But, in a country where health programmes are carried out by state administrations with varying capacities and budgets, public health experts quietly acknowledge that there is a much longer struggle ahead.
In the hamlet of Jairampur — on a highway a few kilometres away from Chaubey’s home, Nirmala Devi Sharma and Urmila Devi, knock at the door of Sita Devi, a 35-year-old housewife and mother of three. Many Indian women use the moniker Devi, which means ‘little goddess’, as an honorific or instead of a surname.
Nirmala is a village-level government health worker, whose normal job is to promote prenatal care and childhood vaccination and to encourage women to give birth in healthcare facilities instead of at home. Urmila runs the local anganwadi, a no-frills childcare centre where young children and mothers receive nutritional supplements.

Nirmala (left) and Urmila (right) are two of the health workers employed to carry out the state's mass drug administration programme
But on this hot spring morning, the two women are foot soldiers in a mass drug administration campaign in Uttar Pradesh’s Bhadohi district, also known as Sant Ravidas Nagar. It is one of the many areas in India where lymphatic filariasis is entrenched in the local community, although most people who harbour the parasite do not know it.
The women’s task for the week is to go door-to-door, distributing the deworming drugs DEC and albendazole for free to every family — and, ideally, to ensure the medicines are taken promptly.
But Sita Devi, who already knows both women, is hesitant: “What kind of disease is filaria anyway?”

Sita Devi (top left and below) is suspicious about the drugs Urmila is bringing
Nirmala describes the distinctive elephant foot. Sita nods in recognition but remains reluctant to take the pills. “What if there are any complications?” she asks. Nirmala is firm: “I told you, there is no problem,” she says. “This is basically to kill the worms.”
Finally, Sita agrees. The health workers reach into a large jar of pills and count out the medication for her, her husband and her two older children. But the pills are not supposed to be taken on an empty stomach and Sita wraps them in small scraps of paper, saying she has not yet had breakfast.
It is unclear whether she will take them at all. “I’ll come back tomorrow — I’ll ask her,” says Nirmala, as she makes a notation with white chalk on the door frame of the house to show she has visited. “I will ask her to show me where the wrappers are.”
As the two women move from home to home through the long, hot day, they meet similar problems. Uttar Pradesh’s mass drug administration campaign was held at short notice, so there was no advance groundwork carried out to explain to people what they should expect. Nirmala and Urmila, who have some high school education, struggle to persuade sceptical locals of the necessity of taking the pills.
Some people swallow the drugs immediately — and give them to their children. But most set them aside for later, citing empty stomachs.
Patients who have the active microfilaria in their bodies often experience fever, muscle pains, headaches and vomiting after taking the drugs — a reaction caused by the death of the baby worms. Typically, these side-effects subside after one or two days but, if not they are not warned about the side effects, people may believe the drugs made them sick.

After she has delivered the medication, Urmila marks the door of each house with white chalk
Mohammad Akram is a carpet trader in his sixties, who lives in a modern second-floor flat with a large television in Jairampur, directly above a workshop where dozens of men are making rugs.
“A lot of people are very nervous and don’t want to take the medicine, but these lovely ladies have convinced them,” Akram says. Urmila interjects, “Uncle, please have your medicine,” she asks, using the respectful term often applied to older men in India. But he refuses: “I’ll have it later.”

Urmila tries to persuade carpet trader Mohammad Akram to take the drugs
Suddenly a woman of similar age enters in the room. Offered the pills by the two health workers, Asma Begum quickly consumes them and then explains that she does not live in the house, but merely works there. “OK, then don’t take these pills again when somebody comes to your house later,” she is told.
Akram’s son, Tariq, asks whether the pills are safe for diabetics like his father. The two women, who had only a single day of training for their task, are not sure. Finally they decide no, since they were told the pills should not be taken by anyone using ‘other medicine’. The younger man chides them. “Not everyone will ask you,” he says. “You should inform them.” In fact, doctors say diabetics can, and should, take the deworming drugs.

The pills consist of two deworming drugs, DEC and albendazole, and are handed out free to every family
Urmila says that public acceptance of the medicine seems to have increased over the years. “This is the third time we are doing this,” she says. “Most people know what this is about.”
But some families refuse even to hold the pills in their hands, especially in Muslim areas, where an ingrained suspicion of the government and its motives runs deep.
“If we [catch] the disease, we will get treated,” says Saima Begum, as she refuses the pills. “But we don’t want to take this. We don’t trust government medicine.” Her husband, Niyaz Ali, another carpet trader, says he had no advance notice of the campaign and nor were any prominent Muslim community leaders involved to reassure the skittish population.
“If people suddenly turn up at your door and tell you to take some medicine, how do you know what it is?” says Ali. “How do you know the medicines are good — and not expired? In this area, people are suspicious of these kinds of medicines. Some people take them; some don’t. We are not too sure why people like us need it.”
At the other end of the country in the southern state of Kerala, the district of Alleppey used to endure one of the highest rates of lymphatic filariasis in India, with as much as 8 per cent of the district’s population infected in the 1970s.
The area, nestled between the Vembanad lake and the Arabian Sea, has an extensive network of canals linking inland areas to what was once a busy port. The canals — many which have fallen into disuse and are choked with water plants — are ideal breeding grounds for the culex mosquito, which spreads the disease.

Canals in Alleppey are ideal breeding grounds for mosquitoes carrying the parasites
“If you said you were from Alleppey, people would look not just at your face, but at your feet,” says Dr Suma Krishnasastry, head of the department of medicine and principal investigator of the filarial research unit at Alleppey city’s TD Medical College. But today, the situation in Alleppey offers hope that India can stop lymphatic filariasis from spreading to the next generation.
The district started experimenting with mass drug administration in the late 1990s, as a pilot scheme for the rest of the country. At first, the effort hit familiar obstacles: public reluctance to take the drugs and the inability of poorly trained volunteers to explain the medicine’s benefits.

Dr Suma Krishnasastry talks to a patient at Alleppey’s TD Medical College
“The people were not aware why they should take the drugs,” recalls Dr Krishnasastry. “Everybody was reluctant to take drugs when they don’t have the swelling. Nobody knew what to do — even doctors and nurses. There was a lot of writing in the newspapers against the drugs.”
State officials gradually stepped up public awareness campaigns, as they expanded mass drug administration to other districts in the state. Politicians and celebrities talked about the safety and necessity of deworming drugs and patients were also drafted in to help. On the ground, health workers were better trained. Volunteers distributed drugs at bus stations, churches and temples to ensure no one was missed out.
The work paid off. In 2013, blood tests of children living in erstwhile microfilaria hotspots in Alleppey showed the presence of parasites was less than 1 per cent.
Today, mass drug administration has stopped in the area and Alleppey, as well as another eight districts in Kerala, are undergoing a four-year surveillance period to find out whether the cycle of transmission has finally been broken. If so, these areas could be declared effectively filaria-free — that would be a tremendous victory for the local public health system and an inspiration for other Indian states that are lagging behind.
Government doctors in Kerala are now focusing on teaching patients with advanced stages of the disease how to take care of their affected limbs — keeping them clean and treating any wounds promptly with antibiotic ointment, so as to reduce the frequency of the paralysing acute infections and further deformities.
“We are getting towards the endgame. There should be a massive education and awareness campaign,” says Dr Krishnasastry. “People need to understand this is for the children of the next generation. They should not be suffering a horrendous malady like this.”
Dr P Jambulingam is director of the Indian government’s Vector Control Research Centre, which provides technical support to the national campaign against lymphatic filariasis.
He says that while progress in states like Kerala is reason for optimism, there are still about 30 districts in other parts of the country that are struggling. For the campaigns to succeed, Jambulingam says, at least 65 per cent of the community in an endemic district needs to take the drugs each year.
“The main challenge is how we can [make sure] people actually consume the drugs,” he says.
The Indian Council of Medical Research is currently testing a new three-drug regimen in one district of the state of Karnataka to see whether it is more effective and can work in a shorter time, he says, although it could be a year before that study is complete.

Shobha lives with her family in Alleppey. She has had lymphatic filariasis since she was a child
Even if India is able to stop the spread of lymphatic filariasis in the next few years, the country will remain home to millions with advanced stages of the disease and incurable symptoms, for whom intervention has come too late.
Shobha AS, who lives in Alleppey, was nine when her left ankle began to bloat. By the time she was 12, her right leg had also started swelling, making it harder and harder for her to get to school. Eventually, she dropped out. “I used to walk to school but, after getting home, my leg was double the size,” she says. “The doctor advised me to stop schooling.”
When she was 21, Shobha’s parents found a local boy who was also suffering from lymphatic filariasis and suggested a marriage, but Shobha refused the match, saying she did not want to be responsible for children. “I told them, ‘Now you are taking care of me, but will you take care of them too?’”
Shobha talks about how her symptoms developed over time
Today, aged 43, Shobha lives with her mother, her sister and brother-in-law and her niece. Her brother-in-law, a labourer, is the main breadwinner and her niece, Ammu, works in the back office of a motorcycle showroom.
Shobha works when she can, mostly on plantations that grow tropical fruits, earning around Rs245 (about $4) a day. But her jobs do not last long as she frequently suffers acute infections which can keep her bedridden for a week at a time. She depends on her family for support, and is particularly close to Ammu, who looks after her when she has fever and vomiting from the infections.

Shobha's niece Ammu paints her toenails in the doorway of the family home
When the mass drug administrations were still under way in Alleppey, Shobha, like many other patients, was actively involved, accompanying health workers as they went door-to-door to encourage people to take the medicine. “I was telling them, ‘If you don’t take it, you will have legs like this,” she says.
But with the campaign now over, and work still hard to come by, she is now a frequent visitor to her local temple, often accompanied by Ammu.
“I am praying that nobody will get this disease,” she says.
Credits
Amy Kazmin, reporting
Mansi Midha, photography and video
Additional imagery: Alamy Photo, Getty Images/iStockphoto, Dreamstime.com
Edited by Cordelia Jenkins
Picture editing by Alan Knox
Graphics by Russell Birkett and Cleve Jones
Production by George Kyriakos and Harriet Thorne
© THE FINANCIAL TIMES LTD 2017
All editorial content in this report is created by the FT. The Bill & Melinda Gates Foundation funded our reporting but had no prior sight of the content.